Author: Colleen Connaughton, PT, DPT
I was sitting in my eye doctor’s office when they told me I needed reading glasses.
Not because something was “wrong,” but because my eyes were working harder than they needed to.
The glasses reduce the effort required.
Same task. Less strain. Better efficiency.
That made me pause.
What if we approached fatigue in multiple sclerosis the same way?
Fatigue in Multiple Sclerosis: Are we Framing it Correctly?
Fatigue is one of the most reported and limiting symptoms in people with multiple sclerosis (MS). It directly impacts mobility, participation, and quality of life.
But here’s the shift that’s happening in neurorehabilitation:
Fatigue is not just something to avoid.
It’s something we can manage, influence, and train around.
Emerging evidence supports a different approach. One that focuses on improving efficiency rather than reducing activity.
Exercise and Fatigue: What the Evidence Now Shows
For years, there was concern that exercise could worsen fatigue in MS.
That position has changed.
Systematic reviews and meta-analyses now show:
- Exercise reduces fatigue and improves quality of life, particularly when combining aerobic and resistance training (Du et al.).
- Meeting physical activity guidelines (about 150 minutes per week) is associated with reduced fatigue severity and impact (Abou et al.).
- Aerobic training improves VO2 peak, which reduces the relative effort required for daily activities (Andreu-Caravaca et al.).
This is a critical point clinically:
Improving physiological capacity changes how hard everyday tasks feel.
Where the Gap Still Exists
Even with this evidence, there is a practical limitation:
Many individuals with MS cannot access or sustain traditional aerobic exercise due to weakness, mobility limitations, or fatigue itself.
That creates a paradox.
The very intervention that reduces fatigue is often inaccessible because of fatigue.
Functional Electrical Stimulation (FES): Reducing the Cost of Movement
This is where Functional Electrical Stimulation (FES) becomes clinically relevant.
FES can assist muscle activation through electrical stimulation, allowing movement to occur with less voluntary effort.
Conceptually, this is similar to reading glasses:
- The task stays the same
- The effort required is reduced
This may allow individuals with MS to participate in aerobic activity more efficiently.
FES Cycling and Multiple Sclerosis: What the Research Shows
FES cycling provides a structured way to deliver aerobic training in individuals with neurological impairments.
Current evidence indicates:
- FES cycling is safe and feasible in non-ambulatory individuals with MS and can improve physical activity levels, fatigue, and quality of life (Backus et al.).
- It produces moderate to large improvements in fatigue, cognitive processing speed, and pain symptoms (Pilutti et al.).
- Exercise, including FES-supported exercise, does not increase relapse risk or adverse events in MS populations (Learmonth et al.).
- FES cycling can generate a meaningful cardiorespiratory training stimulus, even in individuals with severe mobility limitations (Edwards et al.).
These findings are consistent with broader FES literature demonstrating improvements in muscle activation, circulation, and functional capacity across neurological populations.
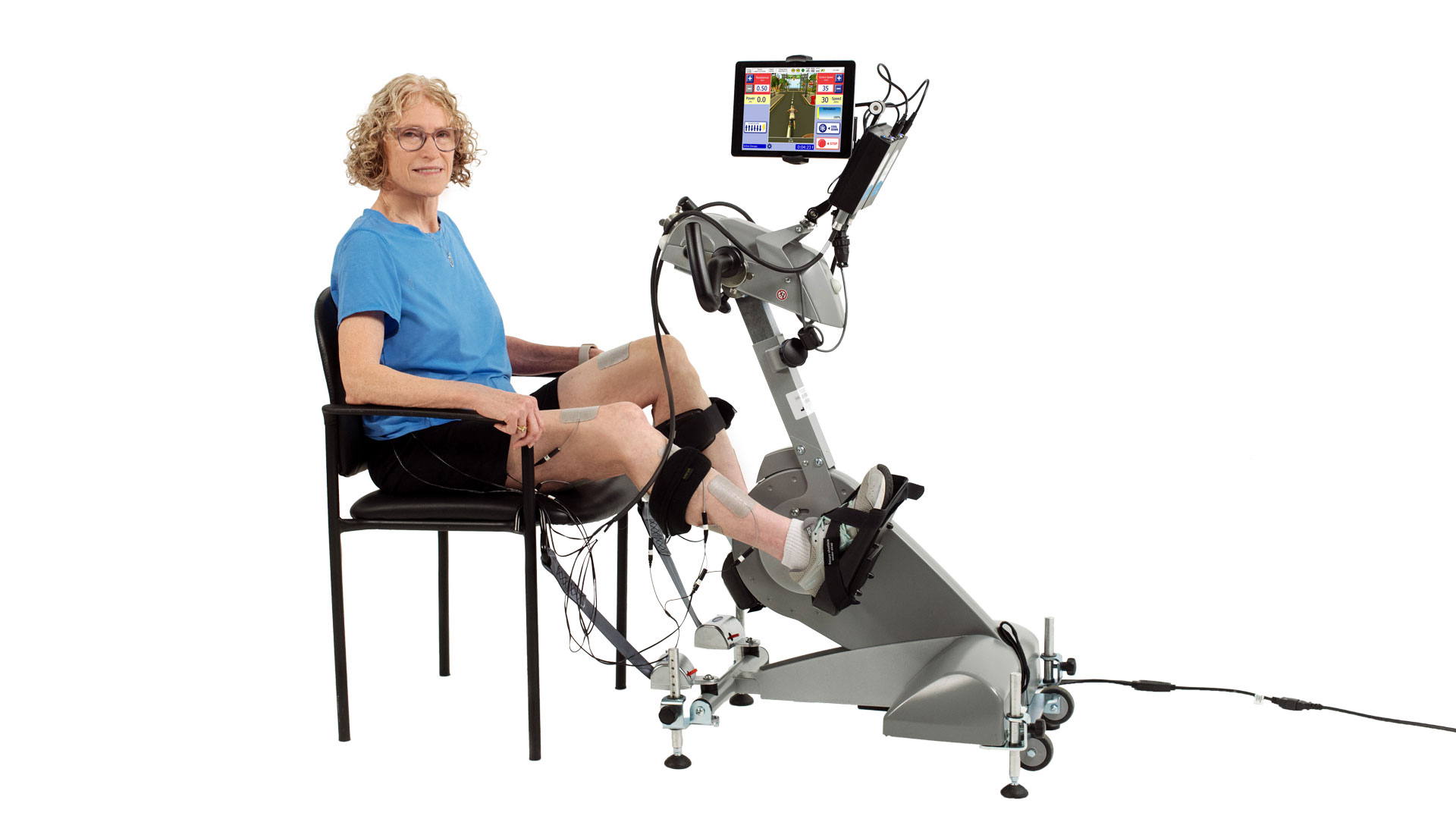
Where RT300 Fits Clinically
The RT300 FES therapy system enables clinicians to deliver coordinated, patterned electrical stimulation during cycling, supporting:
- Muscle re-education
- Relaxation of muscle spasms
- Prevention of muscle atrophy
- Increased local blood circulation
- Maintenance or improvement of range of motion
For individuals with MS, this creates access to repetitive, structured movement that may otherwise be difficult to achieve.
It does not replace exercise.
It helps it happen in a therapeutic way that is meaningful for recovery.
A Shift in How we Think About Fatigue
Fatigue does not always mean stop.
Sometimes it means:
- Reduce the cost of movement
- Improve efficiency
- Increase capacity over time
That shift changes how we prescribe therapy.
Instead of avoiding fatigue, we start asking:
How do we help patients move more efficiently, so they can do more?
A Clinical Question Worth Asking
As we bring March to a close and MS Awareness Month, this is worth reflecting on:
Are we helping patients avoid fatigue…
or helping them move through it more effectively?
Because those are not the same thing.
Fatigue in multiple sclerosis is not just a limitation.
With the right approach, it becomes a modifiable factor in rehabilitation.
FES technology, and systems like the RT300, offer a way to reduce effort, increase access to movement, and support consistent training.
FAQs
What Causes Fatigue in Multiple Sclerosis?
Fatigue in multiple sclerosis is multifactorial and can involve central nervous system dysfunction, impaired nerve conduction, deconditioning, and increased energy cost of movement. It is one of the most common and disabling symptoms in MS.
(Johnson et al.)
Does Exercise Worsen Fatigue in Multiple Sclerosis?
No. Current evidence shows that exercise does not worsen fatigue and can actually reduce it.
Systematic reviews and meta-analyses demonstrate that aerobic and resistance training improve fatigue severity and quality of life in people with MS (Du et al.; Abou et al.).
How Much Exercise is Recommended for People With MS?
Research supports approximately 150 minutes of physical activity per week, including a combination of aerobic and resistance training, to reduce fatigue and improve function (Abou et al.).
Why Does Aerobic Exercise Help Reduce Fatigue in MS?
Aerobic exercise improves cardiorespiratory fitness (VO2 peak), which lowers the relative effort required for daily activities.
This means patients can perform the same tasks with less perceived fatigue (Andreu-Caravaca et al.).
What is Functional Electrical Stimulation (FES)?
Functional Electrical Stimulation (FES) is a rehabilitation technique that uses electrical impulses to activate muscles affected by neurological conditions.
It enables muscle contractions even when voluntary control is limited, supporting movement and neuromuscular activation.
How Can FES Help Manage Fatigue in Multiple Sclerosis?
FES may help reduce fatigue by lowering the effort required to produce movement, allowing patients to participate in exercise more efficiently.
This can help bridge the gap between limited mobility and the need for aerobic conditioning.
What is FES Cycling?
FES cycling combines electrical stimulation with a motor-assisted cycle to produce coordinated muscle contractions in the legs or arms.
It allows individuals with neurological impairments to engage in repetitive, structured aerobic activity.
Is FES Cycling Safe For People With Multiple Sclerosis?
Yes. Research shows that FES cycling is safe and feasible, including in non-ambulatory individuals, with no increase in relapse risk or adverse events (Backus et al.; Learmonth et al.).
What Benefits Does FES Cycling Provide in MS?
Studies have shown that FES cycling can:
- Improve fatigue and quality of life (Backus et al.)
- Improve cognitive processing speed and reduce pain (Pilutti et al.)
- Provide a measurable cardiorespiratory training stimulus (Edwards et al.)
These outcomes support its role in expanding access to therapeutic exercise for individuals with limited mobility.
What is the RT300 FES Therapy System?
The RT300 is a clinic- and home-based Functional Electrical Stimulation cycling system that delivers coordinated, patterned stimulation to activate muscles affected by neurological conditions.
What are the FDA-Cleared Benefits of the RT300?
The RT300 is FDA-cleared to:
- Relax muscle spasms
- Prevent muscle atrophy
- Increase local blood circulation
- Maintain or increase range of motion
- Facilitate muscle re-education
How Does RT300 Support Patients with Multiple Sclerosis?
The RT300 enables repetitive, structured movement and muscle activation, which may help patients access aerobic activity that would otherwise be difficult due to fatigue or mobility limitations.
Can the RT300 be Used at Home?
Yes. The RT300 is designed for both clinic and home use, allowing patients to continue therapy outside the clinic and maintain consistency in their rehabilitation program.
Is the RT300 Exercise Equipment?
No. The RT300 is a prescription medical device that delivers electrical stimulation to activate muscles.
It is used as part of a rehabilitation program under clinical guidance.
Why is FES Important in Neurorehabilitation?
FES provides a way to deliver high-repetition, patterned neuromuscular activation, which is essential for maintaining muscle health and supporting functional recovery in neurological populations.
References
Abou, Libak, et al. “Meeting Physical Activity Guidelines for Persons With Multiple Sclerosis Reduces Fatigue Severity and Impact: A Systematic Review and Meta-Analysis of Randomized Clinical Trials.” Physical Therapy, vol. 105, no. 6, 2025.
Andreu-Caravaca, Luis, et al. “Dosage and Effectiveness of Aerobic Training on Cardiorespiratory Fitness, Functional Capacity, Balance, and Fatigue in People With Multiple Sclerosis: A Systematic Review and Meta-Analysis.” Archives of Physical Medicine and Rehabilitation, vol. 102, no. 9, 2021, pp. 1826-1839.
Backus, Deborah, et al. “Effects of Functional Electrical Stimulation Cycling on Fatigue and Quality of Life in People with Multiple Sclerosis Who Are Nonambulatory.” International Journal of MS Care, vol. 22, no. 4, 2020, pp. 193-200.
Du, L., et al. “Effects of Exercise in People with Multiple Sclerosis: A Systematic Review and Meta-Analysis.” Frontiers in Public Health, vol. 12, 2024, article 1387658.
Edwards, Thomas, et al. “Cardiorespiratory Demand of Acute Voluntary Cycling with Functional Electrical Stimulation in Individuals with Multiple Sclerosis with Severe Mobility Impairment.” Applied Physiology, Nutrition, and Metabolism, 2018.
Learmonth, Y. C., et al. “Safety of Exercise Training in Multiple Sclerosis: An Updated Systematic Review and Meta-Analysis.” Multiple Sclerosis Journal, vol. 29, no. 13, 2023, pp. 1604-1631.
Pilutti, Lara A., and Robert W. Motl. “Functional Electrical Stimulation Cycling Exercise for People with Multiple Sclerosis.” Current Treatment Options in Neurology, vol. 21, no. 11, 2019, article 54.
Johnson, Elise, et al. “Fatigue in Multiple Sclerosis: A Comprehensive Approach to Evaluation and Management.” Practical Neurology, Jan.-Feb. 2024.
Want to learn more about how the RT300 and Xcite2 therapy systems can improve patient outcomes?
Visit restorative-therapies.com to explore how Restorative Therapies supports clinicians and patients in the neurorecovery journey.






